CONGRÈS COMMUN
ASSOCIATION FOR PAEDIATRIC EDUCATION IN EUROPE
ASSOCIATION POUR L’ENSEIGNEMENT DE LA PÉDIATRIE EN EUROPE (A.P.E.E. – A.E.P.E.)
EUROPEAN SOCIETY FOR SOCIAL PEDIATRICS (E.S.S.O.P.)
Bordeaux – France
Sorry, no translation available
Paediatrics: The Changing Needs in Europe
By Dr Viviana Mangiaterra
Regional Adviser for Child Health and Development World Health Organization, Regional Office for Europe
Introduction
The WHO Regional Office for Europe (WHO/EURO) covers 51 countries which are quite different from each other as far as history, culture, economic situation and needs are concerned in public health. At the beginning of the 1980s when the document Targets for Health for All was drawn up to serve as a WHO policy for the European Region, WHO/EURO comprised of only 32 Member States. The Soviet Union was still in existence and the armed conflicts in former Yugoslavia, Chechnya, Tajikistan, Armenia, Albania and in Azerbaijan had not yet broken out. The situation is quite different now; several countries, most of them countries of central and eastern Europe (CCEE) and Newly Independent States (NIS) show much higher infant mortality rates than those initially targeted for the year 2000. Inequities between the different countries of the region remain profound. The socially and economically deprived continue to be the most likely to suffer.
In this Europe of many facets, paediatricians today must adapt themselves to the emerging needs of children and adolescents, while remaining closely attuned to their own society with their new demands.
1. THE NEONATAL PERIOD AND THE FIRST YEAR OF LIFE
WHO/EURO is faced by grave inequities in terms of resources and access to quality perinatal health care services. While in western Europe it is possible to save very premature babies, in many countries of eastern Europe and central Asia lack of a suitable thermometer means that hypothermia cannot always be detected.. Many maternity clinics do not have the basic equipment essential for the care of the newborn. Within the context of large-scale economic crisis, whether this has led to conditions of extreme poverty or merely the necessity to restructure expenditure on health care, appropriate technology is a concept of strategic importance for reducing mortality and morbidity.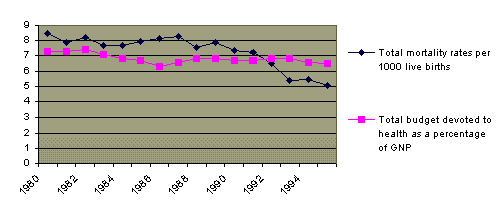
The neonatal period is certainly the most critical period in the life of the young infant. Many instances, mainly from developing countries, show that it is extremely difficult to reduce neonatal mortality rates below a certain level. Experience shows that spending large amounts of money on sophisticated technology is not the answer; a better way is to take preventive measures and to improve the socioeconomic environment of the target population by means of a family-centered and community centered approach. For example, during the past 10 years, Denmark has steadily reduced neonatal mortality rates while keeping its health budget at the same level. In the same way, a comparison between Italy and Finland is interesting, in that while both countries devote the same amount of GNP to health care expenditure, mortality rates in infants under one month in age are twice as high in the former than in the latter. These figures, however, mask some wide disparities between northern and southern Italy; the latter has not yet adopted effective strategies for regionalizaion of care and suffers from serious socioeconomic constraints.
Denmark
Source: Targets for Health for All
The decline in perinatal and neonatal mortality in certain countries, therefore, does not necessarily stem from the application of sophisticated and expensive technology, but is rather due to effective strategies based on a holistic approach to birth, relying on education of women, comprehensive access to prenatal care, improved management of pregnancy and birth and regionalization of perinatal care. Specifically, several countries have obtained excellent results by making early transfer to appropriate hospital centres the rule for women with complications or at risk of very premature delivery. It is less risky of course to transfer babies in utero than after birth, but timely and appropriate action by the health care team is of the essence. This system of speedy transfer is clearly very necessary in such countries as The Netherlands where a large number of women give birth at home, but it is equally important for all births which take place in specialized institutes.
In the European Region, the majority of births take place in hospital. This contributes largely to the quality of care, notably in countries where the infrastructure is not sufficiently reliable to allow for a rapid and effective transfer. On the other hand, such institutionalization of birth has in many cases transformed birth into a medical affair where the physiological and technical aspects outweigh the psychological wellbeing of the mother and the infant. Today we understand more about the emotional needs of the mother, father baby just as we know more about the disadvantages of the medicalization of birth. Birth should be considered as a normal physiological process and not as a pathological one, just as comforting surroundings during delivery and early contact between mother and baby are known to be key components in delivery and care of the newborn. It is, therefore, essential that even in the most minor aspects of care, the rights of the mother and the child should be respected. De-medicalization of birth makes it more humane by giving more attention to the needs of the family, which certainly contributes greatly to successful delivery, although it cannot alone guarantee “safe motherhood”. The technical team comprising pregnancy and delivery must be able to intervene at any moment, although they should as far as possible avoid coming between the mother and her baby.
Breastfeeding is the best investment in the mother-baby relationship, but it is still insufficiently and inconsistently practised in the whole of the WHO European Region, while it is one of the contributors most beneficial to neonatal, infant and child health. In many countries, exclusive breastfeeding during the first six months of life, is rarely practised.
Breastfeeding in Uzbekistan
Not exclusive breastfeeding Exclusive breastfeeding
0 – 3 months 97.6% 4.1%
4 – 6 months 91.5% 0%
7 – 9 months 88.6% 0%
10 – 12 months 77% 0%
Source: Demographic and Health Survey, Ministry of Health, 1996
This is even more serious in the many countries where the main causes of death are still diarrhoeal diseases and respiratory infections for which exclusive maternal breast-milk would effectively decrease their incidence.
The International Code of Marketing of Breast-milk Substitutes prohibits the promotion of these products in the maternity wards, but it is not always respected by the multinational firms in the field of food and agricultural sector who see the former communist countries as new markets for their lucrative profit-making. At the same time, training of health professionals is insufficient in this field and many women still refuse to breastfeed their babies or believe that they are incapable of doing so. There remains, therefore, much ground to cover in order to change practices and mentalities in favour of mother milk.
In the great majority of cases, pregnancy is a normal physiological process which must be de-medicalized and does not require the presence of a highly qualified specialist. That is why the midwife is the best person to give the care needed by the mother and her baby. Her capacity to listen, support and counsel are the key elements to sound care during the process of pregnancy, delivery and postnatal period. In many countries of western, central and eastern Europe, the midwife is not sufficiently valued by the systems of care and it is necessary to give her the benefit of better training and allow her to take more responsibility.
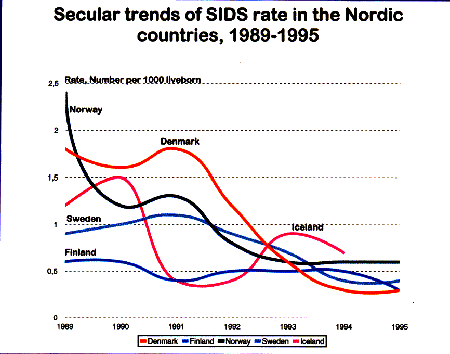
It is now known that the predominant cause of sudden infant death syndrome (SIDS) in infants is the sleeping position . Recent studies have shown that the incidence can be reduced by 60% if the baby is laid to sleep on its back, which is the simplest action to take and is the least costly of all interventions. Other risk factors of SIDS are smoking by parents, insufficient breastfeeding, high temperature of surroundings, and tight swaddling which is widely practised in countries of central and eastern Europe. Very often official figures from these countries includes sudden death of infants under respiratory diseases or accidents. That does not mean that cases of SIDS do not occur, and although they represent a smaller percentage of deaths than in western Europe, they must still be combatted. Much remains to be done to ensure the problem gets the international public health attention it deserves.
In reality, state-of-the-art technology only makes a difference in a tiny portion of deliveries, notably in the case very low birth-weight babies or for those with severe serious congenital defects. Such technology can work miracles in countries which can afford it, but is not always cost-effective on economic or humanitarian grounds.
In western Europe, medical successes lie behind the increase in the number of children suffering complications and multiple handicaps. Ten years ago, some 20% of premature babies survived, 5% of which suffered cerebral palsy. Today, 80% survive, a large percentage of which suffer serious complications, thus increasing the number of brain-damaged babies. Europe therefore accounts for a growing number of infants with tetraparesis, hydrocephalus, epilepsy, severe eye disorders or mental retardation. In order to live and develop, they require not only specialized personnel, but also structured environments adapted to their needs. Europe needs to be prepared for that eventuality.
It may be inquired what the impact of such extremely costly technology on public health will be, particularly as it represents a considerable drainage of funds away from essential care. This is the more serious in that the WHO European Region includes countries with very limited financial resources. The investment choices any society makes have a strategic impact at more than one level and are a factor in determining the viability of health d a determining factor of the viability of the systems throughout a continent.
2. THE FIRST FIVE YEARS OF LIFE
As is the case for the perinatal period, there are considerable inequities in the European Region as regards access of infants to health care. Such inequities exist not only between different groups of countries, but also within countries experiencing economic recession, both in western Europe and more particularly in central and eastern Europe, which have experienced a collapse in household incomes since the onset of the “transition” period.
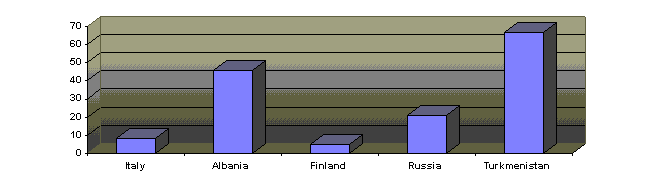
Figure 1. Probability of dying before the age of 5, per 1000: Targets for Health for All
In many countries of central and eastern Europe, children have suffered even more than women and the elderly. Their rate of poverty has increased one-and-a-half times more than that for the country as a whole. The probability of dying before the age of five varies enormously from country to country. These inequities are found when household income is compared to the under-five mortality. Even in countries that have adopted deliberately equitable policies, as in Sweden, a direct connection is found between belonging to given under-privileged social classes and the risk to likelihood of death in childhood. Infant health is, therefore, closely linked to the socioeconomic environment in which the child is raised.
It is, therefore, no surprise that the causes of mortality and morbidity in children under five years of age varies considerably in the countries of the European Region. In western Europe, children die most often from accidents and malignant tumours, while in central and eastern Europe most deaths are caused by infectious disease, immunization-preventable disease and diseases related to nutrition deficiencies. Malnutrition is indeed a growing problem, even if it is of a more moderate order than that seen on other continents. It is common among the under-privileged social classes in all countries of the European Region, but is more widespread in central and eastern Europe and central Asia. It most frequently takes the form of anaemia and iron deficiency.
In the countries where the foremost causes of infant mortality are diarrhoeal and respiratory diseases, it is sometimes necessary to rethink the practice of paediatrics as a whole in order to render it more effective and less costly, in other words to adopt what is called the Integrated management of childhood illness (IMCI). This new approach developed by WHO Headquarters is recognized by many international organizations as one of the most suitable for meeting the needs of poor countries, making it possible to combat the principle causes of death by using protocols of evaluation and simple and effective treatments while avoiding hospitalization of the child. This strategy differs from the vertical approaches used up to now, since it addresses the child as a whole. It is based on prevention and care, improvement of the skills of primary health care professionals, reform of the system of health care and the promotion of family and community responsibility. At the present time, if the prevailing epidemiological situation is taken as the main criterion, nine countries in the European Region are likely to adopt IMCI in the next few years, namely Azerbaijan, Kazakhstan Armenia, Kyrgyzstan, Tajikistan, Turkmenistan, Uzbekistan, Georgia and the Republic of Moldova. The first two have already adopted IMCI as a national strategy. Even though IMCI will affect only a small number of countries in the European Region, it represents an innovative approach to the child, whether sick or well, that gives more attention to the rationalization and regionalization of care. European paediatricians should find it a source of inspiration.
Recently, new causes of morbidity have appeared in the European Region, such as diseases associated with an unhealthy environment. Children are more exposed to pollution than adults because they breathe, drink and eat more in relation to their weight. Children exposed to a polluted atmosphere are more often subject to respiratory problems, using more bronchodilators and having a higher rate of absenteeism from school than those living in a less polluted environment. Even though there are as yet no studies on the long-term effects of such exposure, hospital registers show a peak of admissions of young children suffering from respiratory conditions whenever air pollution rises above certain levels. Eye and skin disorders are becoming more and more frequent, in particular local irritations and allergies. The number of cases of food poisoning is steadily increasing throughout the European Region and infections linked to contaminated water, such as hepatitis A or diarrhoea are among the major causes of illness in the whole eastern part of the continent. In some severe cases, environmental pollution may even slow growth and delay development or cognitive abilities in the child, notably in cases of lead poisoning. Many cases of thyroid cancer have been registered in particularly exposed areas such as that contaminated by the accident at Chernobyl nuclear power station, and some cancers have been linked to exposure of parents to dangerous radiation.
The most affected areas in the European Region are countries bordering the Aral Sea, which are suffering serious ecological disaster as a result of years of unrestricted pollution and mismanagement of soil and water, leading to severe degradation of the environment and consequent repercussions on the life and health of the population. Since the 1960s, the amount of water in the Sea has fallen by 50%, leading to heavy salination of agricultural land. Fishing and farming villages have been practically wiped off the map and hundreds of millions of inhabitants have fled from the disaster areas, creating large groups of ecological refugees living in deplorable sanitary conditions. The water used by the people is heavily polluted with salt, fertilizer and pesticides and the frequency of disease related to poor water quality is high. Less than half of the rural population has access to safe drinking water and nutrition problems are frequent. The destruction of the local ecosystem takes its first toll among women and children, the very young being particularly vulnerable.
The socioeconomic environment is also of prime importance in the psychosocial development of the child, particularly during the first five years of life. In the course of this period, relations with other children and the adult world, within the family, at the day nursery or in school are determining factors in physical, intellectual and emotional development. For the very young, the day nursery has a major role in promoting the child’s health, as it is where for the first time the child experiments with equity, solidarity and respect for himself and others. Unfortunately, in most of the former communist countries, the nurseries and the activity centres that used to be run by the school system or youth movements are now often managed by the private sector and are accessible only to a minority.
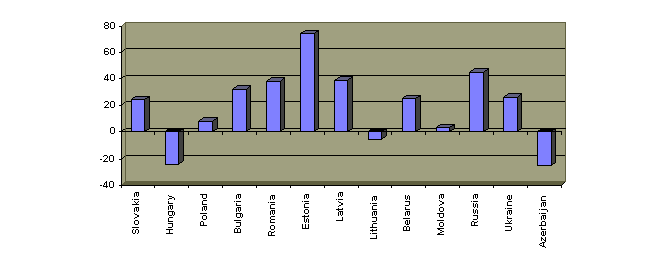
Figure 2. Changes in the rates of children placed in infant homes (percentage change over 1989-1995).
Notes: Slovakia: 1989-94, Poland: 1989-93, Moldova:0-2 years.
Source: UNICEF Children at risk in central and eastern Europe : Perils and promises, 1997.
In the countries of central and eastern Europe, the number of single families has increased rapidly during the past decade, often leaving the women alone to raise their children. Privatization of some health centres, the reduction of social allowances, the fragility of the home environment to the family and the stress linked to the uncertainty of the future are contributory factors to maltreatment of children. The abnormal patters of behaviours common in such contexts are all health risks for the child and the adolescent.
The abuses to which children may fall victim are internationally recognized as violations of human rights and a major public health challenge. It concerns not only sexual abuse but also psychological abuse, negligence and exploitation of child labour, whether in the family, at school, in psychosocial institutions or hospitals. The consequences of such abuse are just as much physical as psychological, and the overall development of the child is profoundly affected, so much so that such children often find themselves socially isolated and without any help to turn to in life’s difficulties.
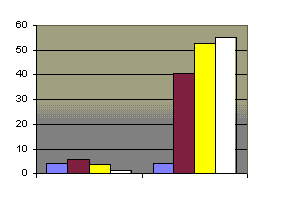
Figure 3: Homicides and purposeful injuries in infants under the age of 1 year,per 1000 Source: Targets for Health for All
Such abuse is certainly not new. The number of cases recorded, however, is steadily increasing, irrespective of whether they concern battered children, victims of sexual abuse or those forced to work in order to meet the needs of a family in economic difficulties. For example, the figures show a steep increase in homicide and injury among children throughout Europe. Even in the Nordic countries. Most cases apparently are of child beating. Such acts are observed among all social classes, but increasing poverty and exclusion has served to emphasize some aspects, notably the emergence of street children, left to their own devices and particularly exposed to maltreatment and prostitution. This is probably happening in the capital cities of western Europe, but in the last ten years, a number of east European cities have become regular centres for the production of pornography. Since these countries have not yet adopted any legislation to prohibit child prostitution or child pornography, those responsible can carry on with their activities with impunity.
It is clear that health professionals have an important role to play, especially in detecting cases of abuse and in the medical treatment of its consequences, and their training needs to be adapted for this purpose. However, regardless of whether maltreatment, malnutrition, respiratory allergies or infectious diseases are in question, a medical approach alone is insufficient. The various professions concerned, whether medical, psychosocial, teaching or legal are all needed to develop a truly intersectoral and multidisciplinary approach in order to improve the overall wellbeing of the child.
3. ADOLESCENCE
All over the world, adolescents behave in ways that constitute a health risk, and Europe is no exception. In a WHO study in 24 countries on the behaviour of school children between the ages of 11 and 15, a large number of the children questioned, with the exception of Sweden, considered they were not in very good health,. They admitted that they were not very happy on the whole, particularly the girls who said they often felt alone and depressed.
The same study showed that accidents are the main cause of mortality and morbidity among adolescents in western Europe. Every year 15-20% of under 14s receive medical care as a result of an accident. Many are hospitalized and some left handicapped. Between 28-42% of the deaths registered are caused by accidents and the figures show that 70% of them concern young boys. Most accidents happen in the home, during sports activities, or at school. On the other hand, road accidents are the most frequent causes of death. Most countries of the European region need to improve the availability and quality of the data they collect with regard to accidents. More detailed research is needed to gain a better understanding of such accidents. It is evident, however, that accidents place a very heavy burden on families and on society as a whole. To combat accidents, large-scale education and information campaigns are needed and legal measures to prevent accidents introduced.
Much experience, notably in western Europe had shown that laws and regulations promoting the safety of young people as well as preventive programmes involving the community as a whole, can reduce the number of accidents considerably.
Adolescents, as a prime target by the fast-food chains, are increasingly likely to have an unbalanced diet, poor in fruit and vegetables and rich in fats and sugar. The practice of slimming diets and the urge to lose weight are widespread, particularly among young girls over 15, who are unfortunately increasingly suffering from serious eating disorders such as anorexia and bulimia. The maintenance of regular meals probably keeps this phenomenon in check, but it is becoming urgent to design education programmes on healthy eating for young people at school and in other places they frequent.
Other high-risk behaviour among young people in Europe are excessive smoking, heavy drinking and drug taking. In the countries of central and eastern Europe, multinationals selling alcohol and cigarettes, attracted by the size of these new markets, aggressive marketing techniques to get young consumers established. adopt vigorous commercialization to gain the youth consumer. Often, the price of alcohol and cigarettes has increased less rapidly than that of basic food commodities which makes these hazardous products even more accessible. Experience shows once more that it is difficult to combat these trends, but money has to be put into information and prevention campaigns and strict national regulations established.
Even worse, drug abuse is more frequent among deprived young people, such as street children or those from ethnic minorities. Figures show those who take drugs do so at younger and younger ages, as in Bulgaria where the first encounter with heroin starts between the ages of 14 and 16. Sniffing of substances such as glue, first takes place around the age of 12. Drug-addiction does not only have adverse effect on development of the neurological system. It also leads to diverse problems such as unprotected sex, unwanted pregnancies, dropping out of school, violence and delinquency.
Minors registered by Internal Affairs Organs (OVD) in Russia by reason
(absolute numbers)
1990 1991 1992 1993 1994 1995
Misdemeanours 245.342 219.040 278.246 320.906 392.364 446.265
Alcohol abuse 122.630 106.219 118.760 162.174 236.378 269.086
Too young to be sentenced 54.635 53.477 66.556 73.946 82.543 88.891
Drug abuse 9.127 7.643 3.402 4.133 5.573 10.813
Others 154.018 147.805 93.058 95.144 120.852 125.644
Total 585.752 534.184 560.022 656.303 837.710 940.699
Source MONEE Database, UNICEF ICDC
Such risky behaviours has led to a rapid increase in the number of young people with sexually transmitted diseases, mainly in the countries of central and eastern Europe. The increase in the number of young people suffering from gonorrhea and syphilis, which increases the risk of HIV infection is disturbing. Among the factors contributing to this alarming development is the lack of information, the spread of prostitution and the difficulty of obtaining condoms because of their high cost.
Lastly, psychosocial problems, violence and suicide, even among the very young adolescents, are the cause of a growing number of deaths or cases of handicap. They are signs of a continent in crisis which no longer allows for a favourable climate in which to flourish. This is particularly true not only in troubled suburbs in western Europe, but also in all urban areas of eastern Europe, where the economic crisis and social tensions have eroded the family stability, parental guidance and confidence in the future.
Faced with these problems, schools are a powerful means to health promotion. In this connection, one of the most interesting initiatives is the European Network of Health-promoting Schools. It was created at the beginning of the 1980s by the WHO Regional Office for Europe, the European Commission and the Council of Europe using an innovative approach to promote health within the school framework. The Network is based on the Ottawa Charter for Health Promotion, aiming to promote intersectorial action. Since its launch, the Network has developed rapidly and had 37 participating countries by 1997. Pilot schools are engaged in promoting health by providing a stable and favourable environment, in which each child is able to live, work, learn and thrive. It mobilizes partnerships between teachers, pupils, parents and the community as a whole. The Network held its first European conference in Greece in May 1997 and has adopted a Resolution of 10 fundamental recommendations which lay the foundation for investing in education, health, and democracy for the future generations.
Undoubtedly, such a school environment makes a positive contribution to the social development and effective wellbeing of young people. An initiative such as the Network of Health-promoting Schools is a model to be followed but large numbers of young people in Europe are completely outside the school system and are left to their own devices on the labour market or on the streets. Another avenue is needed to reach them, such as youth organizations, sports clubs, parents or social workers.
To maximize the health potential of adolescents, action must be channeled largely through education dialogue and communication. This should be done by means of intersectoral and coordinated initiatives, involving not only young people themselves, but also all other players in their emotional environment family and social environment in order better to assist them in becoming responsible for their own health.
CONCLUSIONS
In the WHO European Region, the health of children and adolescents is largely determined by the socioeconomic environment in which they are born and raised. The wide disparities observed between groups of countries are also seen within each society, between the most privileged and the poorest.
In order to reach the goals of Health for All, medical action is unavoidable, but cannot alone lighten the burden of disease. It must respond to the economic constraints of health care systems and provide more equitable access to the determinants of health. Thus, overcoming poverty, health education, prevention of disease and accidents, protection of the rights of the child and its mental balance are all essential factors in advancing better health.
Paediatricians today need to take into account the new needs of the many faceted Europe in which they practice. In order to increase the thrust of their action, they must take on board new models of work and organization, act within the framework of improved partnerships with other professions involved with the young people, acquire new tools such as epidemiology and management of health care services, and take inspiration from the experiences of neighbouring countries. Europe must, therefore, strengthen national and international solidarity and adopt a multisectoral approach to improve the health of those who will build the twenty-first century.
1. Infections, parasitical diseases, acute respiratory infections, influenza
2. Neoplasm, accidents and secondary effects
